Strategic Plan Development
To develop the IHS Strategic Plan FY 2019-2023, the IHS used a process similar to the HHS Strategic Plan FY 2018-2022,[4] including the use of goals, objectives and strategies, environmental scans, Strengths, Weaknesses, Opportunities, and Threats (SWOT) analysis, and workgroup participation.
An IHS-initiated environmental scan reviewed strategic plans of several IHS area and headquarters offices, and other available documents. The SWOT exercise was conducted with IHS executive staff. Informed by these documents and analysis, the IHS developed an initial framework for review and comment of the Strategic Plan by Tribes, Tribal organizations, UIOs, and IHS staff. The IHS first initiated Tribal consultation and urban Indian confer on the IHS Strategic Plan initial framework on September 15, 2017, and formed an IHS Federal-Tribal Strategic Planning Workgroup (workgroup) to review all comments and recommend a list of final goals and objectives for IHS leadership review and approval.
During the initial framework comment period (September 15, 2017 - October 31, 2017), the IHS held listening sessions, presented at Tribal meetings, and held conference calls with Tribal and UIO leaders. Workgroup membership included Tribal leaders or their designees, a representative from the IHS Office of Urban Indian Health Programs, and IHS staff from areas, service units, and headquarters. The workgroup reviewed comments on the initial framework received from 150 Tribes, Tribal organizations, UIOs, and IHS staff. Subsequently, the workgroup met six times over a four-month period to develop their final recommendations on the IHS mission, vision, goals, objectives, and strategies.
The workgroup prioritized strategies by importance, and not all strategies were recommended. Quality as a Business Strategy (QBS)[5] was used as a model for developing the IHS Strategic Plan. Strategies were developed in alignment with defined goals and objectives to continue current operations or improve the Indian health care system. In doing so, the IHS Strategic Plan addresses quality throughout all aspects of its clinical, operational, and administrative operations and creates a plan for improvement across all three areas.
Feedback received from all stakeholders formed the basis of the Draft IHS Strategic Plan 2018-2022 sent out for public comment on July 24, 2018. During the 30-day comment period, which ended on August 23, 2018, the IHS received comments from 30 entities, including Tribes, Tribal organizations, UIOs, IHS staff, and national organizations. The final IHS Strategic Plan FY 2019-2023 reflects changes made to the initial framework based on consideration of all comments received. The IHS Strategic Plan FY 2019-2023 may be accessed through the IHS website at https://www.ihs.gov/strategicplan/.
The IHS intends to identify appropriate performance measures and outcomes to achieve the mission and goals. The IHS is working to develop an implementation process that will include measures to address the strategies and objectives in the IHS Strategic Plan. The IHS will review periodically the agency’s progress in implementation of the IHS Strategic Plan and will provide updates to IHS staff and to Tribal and UIO leaders.
Priorities and Challenges
The IHS has historically established four priorities to guide operations. The IHS Strategic Plan FY 2019-2023 incorporates these priorities and builds on the important work being done throughout the system.
The IHS four priorities are interrelated with the strategic goals of the IHS Strategic Plan FY 2019-2023:
- People – Recruit, develop, and retain a dedicated, competent, caring workforce collaborating to achieve the IHS mission.
- Partnerships – Build, strengthen, and sustain collaborative relationships that advance the IHS mission.
- Quality – Excellence in everything we do to assure a high-performing Indian health system.
- Resources – Secure and effectively manage the assets needed to promote the IHS mission.
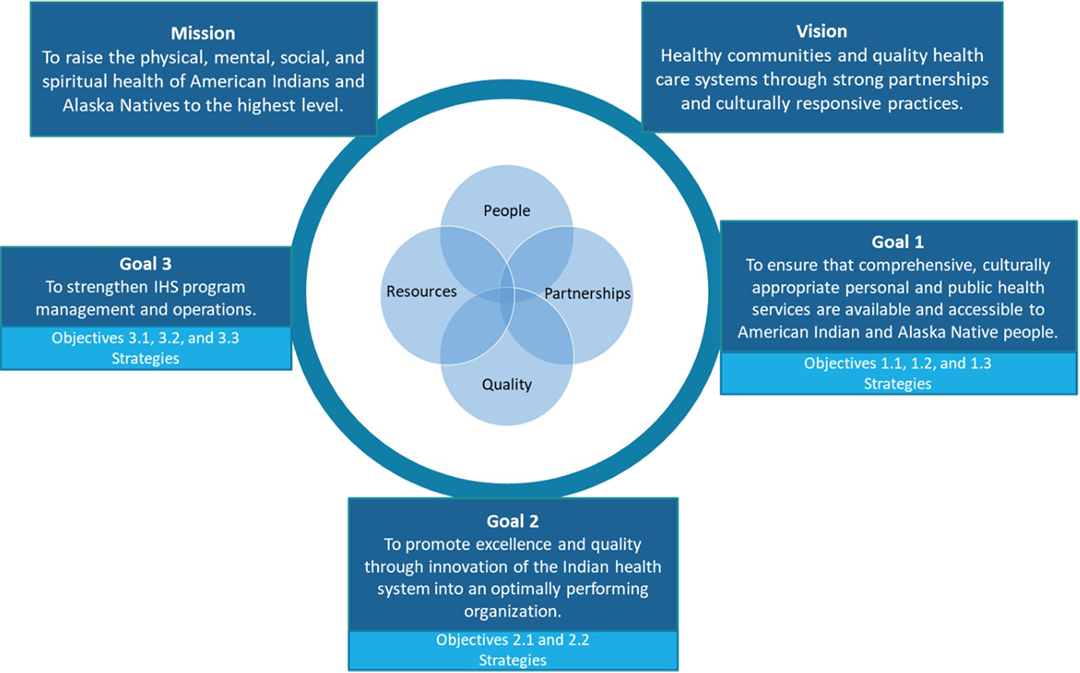
Figure 1. The IHS Strategic Plan and the IHS Four Priorities
The AI/AN population continues to face health disparities in comparison to the national population. Over the past two decades, there have been some important health improvements, such as reduced mortality rates from tuberculosis and heart disease, among others. However, the infant mortality rate for AI/ANs is 26 percent higher than the national rate,[6] and AI/ANs are three times as likely as the overall population to have diabetes.[7] American Indian and Alaska Native populations also have disproportionately high rates of suicide, unintentional injuries, and drug overdose deaths. The IHS Strategic Plan aims to strengthen the overall health status of the AI/AN population.
In recent years, the agency has faced challenges related to access to care, quality of care, and program management and operations. The IHS Strategic Plan includes three strategic goals focused on access, quality, and management and operations.
Access: Many facilities operated by the IHS and Tribes are located in rural or remote settings and may be unable to provide comprehensive health care services and/or acute and specialty care services. To help meet the health care needs, the PRC program purchases services from private health care providers for eligible patients. Although PRC funding may meet the full patient need in some IHS areas, funding may not be sufficient to meet the need in others. Some facilities also face longstanding challenges in recruiting and retaining essential staff, ensuring access to needed care and training resources, and maintaining clinical proficiency of professional staff. Recruitment and retention challenges are attributable to a variety of factors that include, but are not limited to, the remoteness of some IHS facilities, rural reservation communities, aging IHS facilities and medical equipment, housing shortages, limited access to schools and basic amenities, limited spousal employment opportunities, and competition with higher paying public and private health care systems. The IHS Strategic Plan Goal 1 aims to address some of these challenges.
Quality : Assuring that IHS hospitals and clinics are accredited is a high priority for IHS. Meeting Medicare standards also allows IHS facilities to be reimbursed for all eligible Medicare and Medicaid services. The IHS monitors federal hospitals through area offices, which have access to information about the quality of care and oversight through a governing body process. Staffing and funding shortages at area offices also have an impact on the clinical support and guidance provided to service units. The IHS is working to strengthen organizational capacity to improve our ability to meet and maintain accreditation of IHS direct service facilities, align service delivery processes to improve the patient experience, ensure patient safety, establish agency-wide patient wait time standards, and improve processes and strengthen communication for early identification of risks.
Within the Indian health care system, quality is also impacted by rising costs from medical inflation, population growth, increased rates of chronic diseases, and aging facilities and equipment. These challenges may be heightened at facilities located in rural, remote locations. The Indian health care system is also challenged with balancing the needs of patients served in IHS, Tribal, and UIO health programs. Goal 2 aims to address these challenges.
Management and Operations : The Indian health care system continues to face management and operational challenges in the years ahead. Communication and collaboration across the system requires improvement and managers need tools and resources to make data-driven decisions. Additionally, while some AI/AN communities have modern IHS hospitals and ambulatory facilities, the average age of IHS facilities is 36 years. Many IHS and Tribal health care facilities and UIOs are operating at or beyond capacity, and their designs may not be efficient in the context of modern health care delivery. Information Technology also continues to be a major concern with rising costs and increased security threats. Goal 3 aims to address these challenges.
[4] A crosswalk of the HHS Strategic Plan FY 2018-2022 and IHS Strategic Plan FY 2019-2023 goals and objectives is available in Appendix A.
[5] QBS is a leadership framework and set of activities to help organizations prepare to participate in system transformation and continuous quality improvement. QBS guides strategic planning through a vision of the system that operates in its present condition (maintaining operations that achieve goals and objectives) and improves to meet new needs through redesign of existing conditions or design of new processes, products, or services. QBS helps leaders plan to operate the system and plan to improve the system.
[6] U.S. Department of Health and Human Services, IHS. (2014). Trends in Indian Health: 2014 Edition. Retrieved from: https://www.ihs.gov/dps/publications/trends2014/ .
[7] Data comparing the AI/AN population to the U.S. general population are documented and updated annually by the IHS . As of April 2018, the most current IHS mortality data available is from 2009-2011. AI/AN mortality data accounts for misclassification of AI/ANs on death certificates and there is a time lag in producing IHS mortality data.


