COVID-19 Rebound After Paxlovid Treatment
The Centers for Disease Control and Prevention (CDC) released a Health Advisory Network (HAN) Health Advisory on the potential for recurrence of COVID-19 or ?COVID-19 rebound.?
Recent case reports document that some patients with normal immune response who have completed a 5-day course of Paxlovid for laboratory confirmed infection and have recovered can experience recurrent illness 2 to 8 days later, including patients who have been vaccinated and/or boosted. Both the recurrence of illness and positive test results improved or resolved (median of 3 days) without additional anti-COVID-19 treatment. Based on information from the case reports, COVID-19 rebound did not represent reinfection with SARS-CoV-2 or the development of resistance to Paxlovid; also, no other respiratory pathogens were identified among known cases.
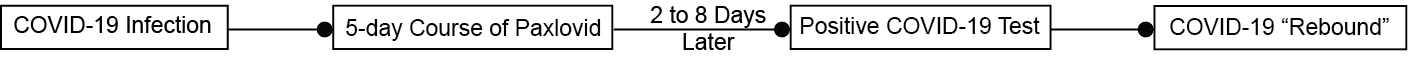
There was no increased occurrence of hospitalization or death.It remains unknown whether the likelihood of possible transmission of infection during COVID-19 rebound differs from the likelihood oftransmission during the initial infection, therefore patients with COVID-19 rebound are encouraged to follow CDC’s guidance on isolation .
Recommendations for Healthcare Providers
For patients with COVID-19 rebound
- There is currently no evidence that additional treatment for COVID-19 is needed for COVID-19 rebound. Based on data available at this time, patient monitoring continues to be the most appropriate management for patients with recurrence of symptoms after completion of a treatment course of Paxlovid.
- Advise people with COVID-19 rebound to follow CDC’s guidance on isolation and take precautions to prevent further transmission. Patients should re-isolate for at least 5 days. Per CDC guidance, they can end their re-isolation period after 5 full days if fever has resolved for 24 hours (without the use of fever-reducing medication) and symptoms are improving. The patient should wear a mask for a total of 10 days after rebound symptoms started.
- Consider clinical evaluation of patients who have COVID-19 rebound and symptoms that persist or worsen.
- Healthcare providers are encouraged to report cases of COVID-19 rebound to Pfizer after Paxlovid treatment using the following online tool: Pfizer Safety Reporting and to FDA MedWatch. Instructions for reporting can be found online at the NPTC Pharmacovigilance website. Please be sure to add “IHS” to section G (Reporter) of the report.
For patients just diagnosed with COVID-19
- Healthcare providers should counsel patients on available COVID-19 treatment options, particularly for those patients at increased risk of developing severe COVID-19.
- Paxlovid should be considered for any patient who meets the eligibility criteria. For information on Paxlovid eligibility, refer to FDA’s Fact Sheet for Healthcare Providers .
- Due to the potential for severe drug-drug interactions with the ritonavir component of Paxlovid, it is strongly suggested that healthcare providers not experienced in prescribing this drug refer to the Fact Sheet for Healthcare Providers , the Paxlovid Patient Eligibility Screening Checklist Tool for Prescribers, and the NIH Statement on Paxlovid Drug-Drug Interactions . Healthcare providers can also contact a local clinical pharmacist or infectious disease specialist for advice.
- For further information on the use of Paxlovid, CDC recommends healthcare providers continue to closely follow NIH’s COVID-19 Treatment Guidelines , the Assistant Secretary for Preparedness and Response Public Health Emergency COVID-19 Therapeutics site , and IDSA’s Guidelines on the Management of Patients with COVID-19 .


