Function-Based Objectives
Often times, a chronic pain patient is asked to rate his or her pain on a scale of 1 to 10, with 10 being the worst pain. However, using a numerical scale alone can have a couple of drawbacks. For one thing, different patients have different pain tolerances; one person's "3" could be another person's "7." The other problem is that a chronic pain patient might report a sizable reduction in pain and at the same time be bedridden, which is not a success.
A function-based treatment strategy measures a patient's progress not in pain relief, but in his or her ability to function better in life. Functional goals would include sleeping, walking, working, connecting with friends, etc. A functional scale would start with only one or two activities affected on the low end and finish with a number of activities affected at the high end. For example, in the sample scale shown below, the scale starts with just one function adversely affected — enjoyment — and then adds one more function with each step up the scale, ending with seven functions adversely affected as pain worsens: enjoyment, work, mood, activity, sleep, walking, and relationships.
Activities Limited by Pain
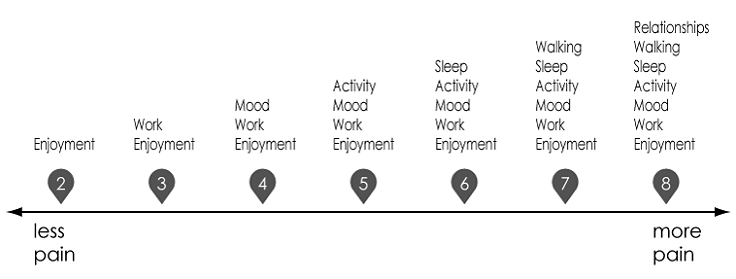
Source: Adapted from Responsible Opioid Prescribing: A Physician’s Guide by Scott M. Fishman.
With the function-based paradigm, a chronic pain patient may not report pain reduction; but, if he or she has started walking, sleeping normally, and engaging in daily activities, then progress has clearly been made.
It is important to understand that progress in pain reduction and a return to activities is slow, lasting months or years. Gains are incremental, literally step by step. Sometimes, the patient hits a plateau.
The Defense and Veterans Pain Rating Scale (DVPRS)
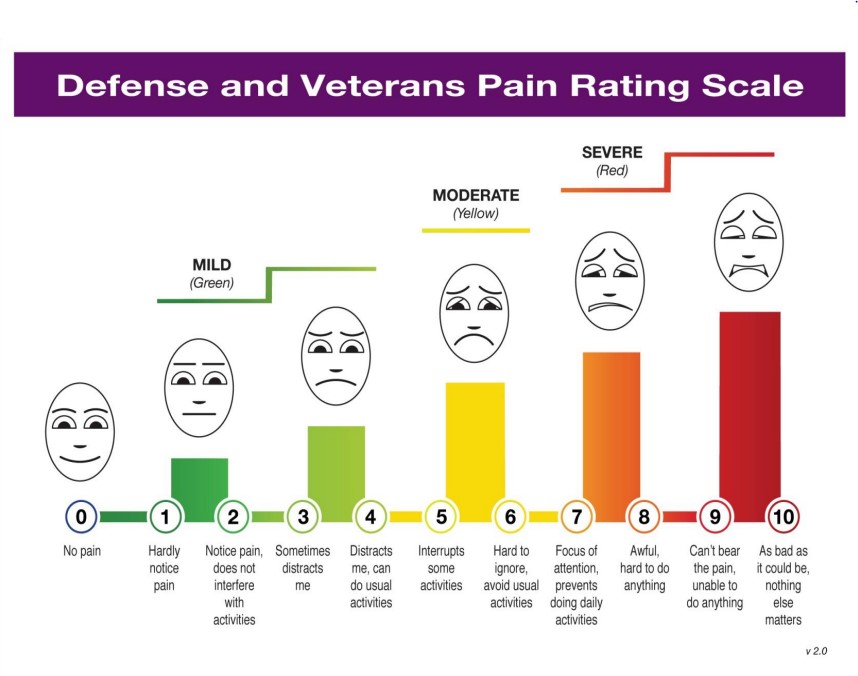
The Defense and Veterans Pain Rating Scale (DVPRS) [PDF - 484 KB] , shown below, is a visual tool clinicians use to facilitate self-reported pain diagnoses from patients, and improve the pain conversation between the patient and the clinician. Designed to improve communication and documentation of pain intensity levels among military personnel and veterans, it may also be used for all people suffering from a pain diagnosis.
The main part of the tool is a color coded graphic showing facial expressions, and divides pain into three ranges: mild, moderate, and severe. Each pain range is associated with specific colors and numbers; each number is then associated with specific descriptions detailing how the pain impacts one's life and daily activities. This allows the patient to determine where they fall on the scale based on evaluating their current activity limitations, in hopes to spark positive conversation between patient and clinician in order to determine an individualized treatment plan with patient-specific goals of therapy.
References
The Defense and Veterans Pain Rating Scale (DVPRS)
Fishman, MD, Scott M. Responsible Opioid Prescribing: A Physician’s Guide. Washington, DC: Waterford Life Sciences, 2007. pp. 34–42.


