Reimbursement Rates
Introduction
On an annual basis, the Indian Health Service (IHS) calculates and publishes, in the Federal Register, calendar year reimbursement rates. The rates are often referred to as the All-Inclusive Rates (AIRs), Office of Management and Budget (OMB) rates, or encounter rates. For the purpose of this guide, these rates will be referred to as the AIRs.
The AIRs are established by IHS based on annual cost reports prepared by IHS’s contractor. IHS reviews the cost reports and upon completion of the review, IHS submits recommended rates to OMB for final approval through HHS and CMS Upon approval by the OMB, the approved rates are published in the Federal Register and IHS systems can be updated with the new rates for billing. The CMS Medicare contractor and State Medicaid agencies are notified when the rates are published so that systems can be updated to pay the new rates.
Due to the higher cost of living in Alaska, separate rates are calculated for Alaska and the Lower 48 States. The four rate categories for Alaska and the Lower 48 States are as follows:
- Inpatient Hospital Per Diem Rate
- Excludes Physician/Practitioner Services
- Outpatient Per Visit Rate (Excluding Medicare)
- Includes Physician/Practitioner Services
- Includes dental, optometry and other Medicaid allowable services.
- Outpatient Per Visit Rate (Medicare)
- Excludes Physician/Practitioner Services
- Medicare Part B Inpatient Ancillary Per Diem Rate
- Excludes Physician/Practitioner Services
Facilities whose costs are included in the AIR are subject to change on an annual basis. The decision to include or exclude a facility is based on its specific facility type in a given year.
The primary sources of information included in the AIR calculations include:
- the annual Medicare cost reports (for each included facility, area office and IHS headquarters),
- IHS inpatient days (IHS annual 202 report),
- IHS outpatient visits (IHS annual 1A report), and
- IHS ancillary study.
Each of these listed sources of information is discussed in detail below.
IHS Part A hospitals are required to electronically file their Medicare cost reports in accordance with 42 CFR 413.24(f)(4)(ii).
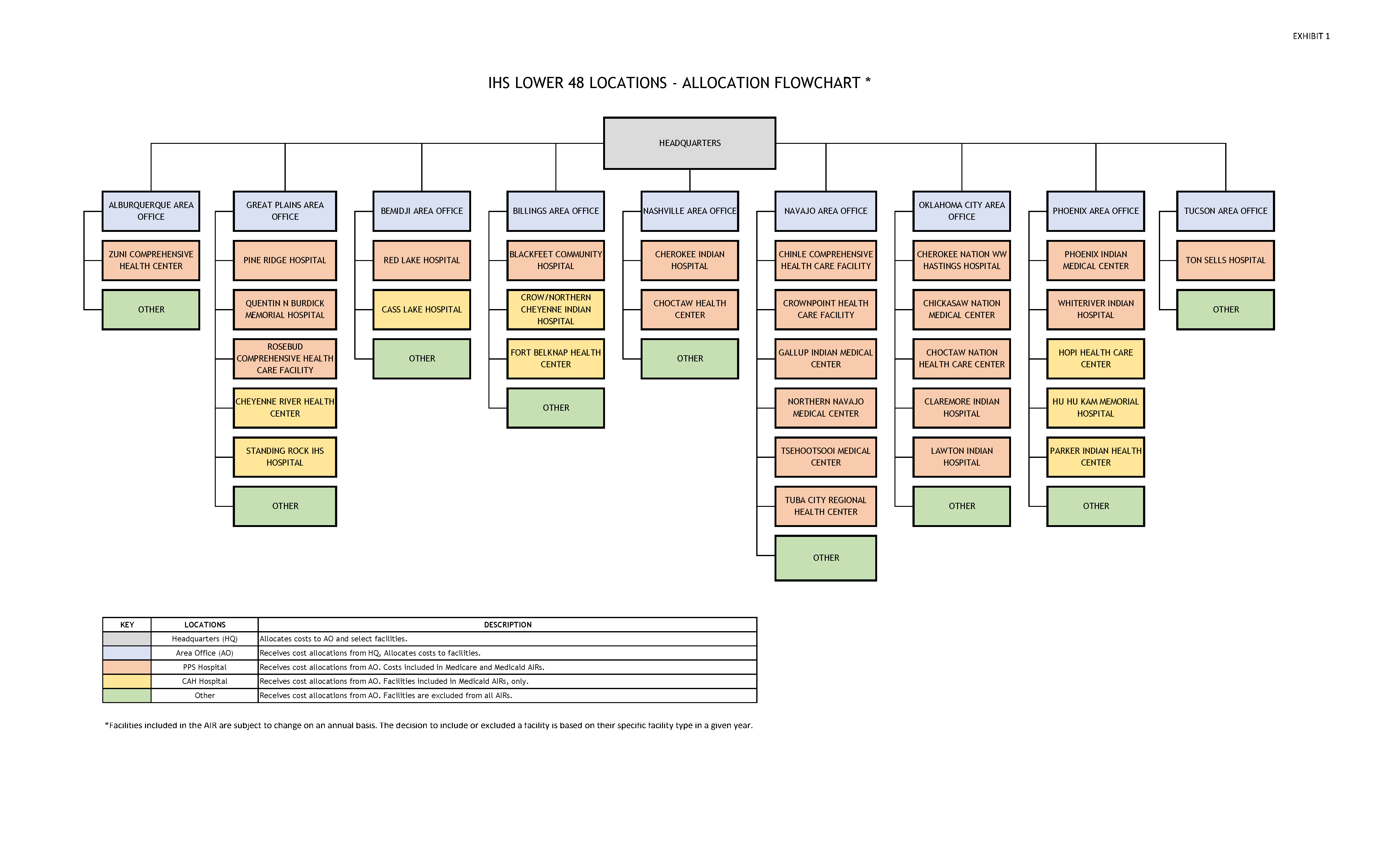
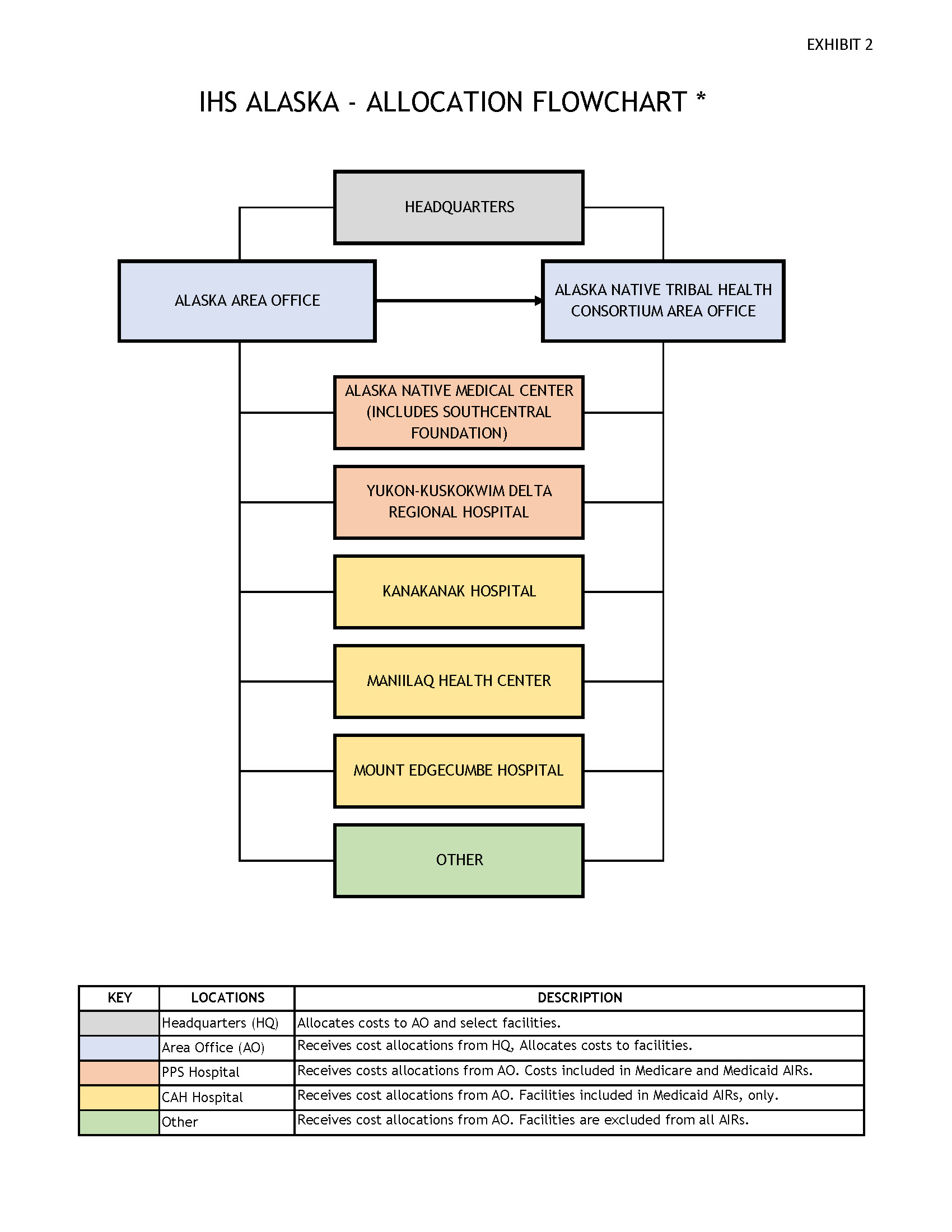
Cost reports are prepared for IHS headquarters, all area office locations, and all participating hospitals (see Exhibit 1 and Exhibit 2 for a complete list of facilities included in the CY 2023 calculations). The cost reports are designed to capture the allowable direct and indirect costs of IHS headquarters, each area office and each hospital including their related hospital-based clinics.
Inpatient days are captured on an IHS annual 202 report that includes hospital inpatients and swing bed patients. Adjustments are made to remove non-acute days and related costs. Non-acute days relate to the portion of an inpatient stay that is not medically necessary.
IHS defines a hospital “outpatient” (OP) as a person who has not been admitted by the hospital as an inpatient but is registered on the hospital records as an outpatient and receives services from the hospital.
In order to allocate ancillary costs between the inpatient AIR and outpatient AIR, an ancillary rate is derived from an ancillary study. The ancillary study is designed to determine the average amount of ancillary resources of an inpatient day compared to the average amount of ancillary resources of an outpatient visit. The ancillary rate is used to calculate the average ancillary cost per inpatient day and ultimately the ancillary costs applicable to the inpatient AIR.
Annual AIRs are calculated for facilities located in the lower 48 States (see Exhibit 1 for a complete list of facilities included), and for facilities located in Alaska (see Exhibit 2 for a complete list of facilities included). The following is a list of all AIRs calculated for both the lower 48 States and Alaska:
| LINE DESCRIPTION | EXAMPLE YEAR | REF |
|---|---|---|
| Routine Costs | $300,000,000 | A |
| IP Ancillary Costs | $77,962,577 | B |
| Total Routine and IP Ancillary Costs | $377,962,577 | C = (A+B) |
| Total IP Days | 100,000 | D |
| $3,779 | E = (C/D) |
| LINE DESCRIPTION | EXAMPLE YEAR | REF |
|---|---|---|
| OP Ancillary Costs | $1,422,037,422 | A |
| Provider, Dental, Optometry, and Other Medicaid costs | 575,000,000 | B |
| Total Medicaid OP Costs | $1,997,037,422 | C = (A+B) |
| Billable OP Visits for Medicaid | 3,200,000 | D |
| Optometry and Dental Visits | 125,000 | E |
| Total Billable OP Visits | 3,325,000 | F = (D+E) |
| $600 | G = (C/F) |
| LINE DESCRIPTION | EXAMPLE YEAR | REF |
|---|---|---|
| OP Ancillary Costs | $1,214,754,098 | A |
| Total Billable OP Medicare Visits | 2,000,000 | B |
| $607 | C = (A/B) |
| LINE DESCRIPTION | EXAMPLE YEAR | REF |
|---|---|---|
| Total Ancillary Costs | $1,300,000,000 | A |
| Adjusted IP Days | 1,220,000 | B |
| $1,065 | C = (A/B) |
Please note that the Centers for Medicare & Medicaid Services (CMS) has issued a Final Rule to continue to pay an add-on to the Medicare Outpatient Per Visit Rate listed below for certain high-cost drugs for people with Medicare who receive care at IHS or Tribal hospitals for CY 2026. See 90 FR 53448, (November 25, 2025). The high-cost drugs qualifying for this add-on payment for CY 2026 are listed in Addendum Q to this Final Rule, available at https://www.cms.gov/medicare/payment/prospective-payment-systems/hospital-outpatient/regulations-notices/cms-1834-fc.
Please contact CDR Tracy Sanchez, Acting Director, Office of Resource Access and Partnerships at tracy.sanchez@ihs.gov.